| |
Choice and Use of Taxanes |

EDITOR’S COMMENT
Docetaxel is being utilized somewhat more frequently than paclitaxel in the adjuvant setting. Most physicians have prescribed a taxane in the therapy of a node-negative patient, but only in a minority of patients — most likely those at higher risk.
Related Comments from Research Leaders
Adjuvant AC followed by docetaxel is being used by many oncologists in practice, but we don’t know how it compares to dose-dense AC followed by paclitaxel. Indirect evidence suggests that docetaxel is better than paclitaxel. A direct comparison between paclitaxel and docetaxel administered every three weeks in patients with metastatic breast cancer, presented at the 2003 San Antonio Breast Cancer Symposium, demonstrated a survival advantage for docetaxel.
The data from the randomized Intergroup adjuvant trial will be reported in the next 18 to 24 months, and I will wait to draw a final conclusion at that time. In that trial, which is closed to accrual, patients were randomly assigned to either paclitaxel or docetaxel and to either an every threeweek regimen or a weekly regimen. I believe paclitaxel may be better when administered weekly, and docetaxel may be better when administered every three weeks. It will be interesting to see how weekly paclitaxel will compare to every three-week docetaxel.
— I Craig Henderson, MD
At ASCO 2003, I presented the first planned analysis of an adjuvant trial comparing four cycles of docetaxel and cyclophosphamide (TC) to four cycles of doxorubicin and cyclophosphamide (AC). The trial was underpowered with a total of 1,016 patients and approximately 500 patients per treatment arm.
The patients were pre- or postmenopausal and had either node-negative or node-positive disease. At 42 months of follow-up, there were fewer recurrences in the patients treated with TC than those treated with AC.
We had previously demonstrated that TC was somewhat better tolerated than standard AC. Patients treated with TC had some of the usual docetaxel-related side effects (eg, arthralgias, peripheral neuropathy), but they had less mucositis, anemia, nausea and vomiting.
I use adjuvant TC for patients as an alternative to anthracycline-based regimens and I’ve used TC in patients with heart disease or those previously treated with doxorubicin. I see little reason to use CMF. The TC regimen has no cardiac toxicity or long-term toxicities at 42 months.
For many patients with node-negative disease, four cycles of adjuvant AC is standard treatment, but if there were any hesitancy to use it because of heart disease or other issues, I would use four cycles of TC.
— Stephen E Jones, MD
When NSABP-B-30 was designed in 1997, taxanes were not routinely used in the adjuvant setting. Many of the investigators, including myself, believed that docetaxel was the most active agent in metastatic disease, and that it should be investigated in the adjuvant setting, which is why we included it in all three arms of B-30.
We also wanted to compare the various durations of treatment, so while the AC followed by docetaxel arm is a sixmonth treatment, the other arms are shorter in duration.
The NSABP data showed four cycles of AC was effective, and we felt that four cycles of AT or TAC would also be effective. Perhaps with hindsight, based on the TAC data, it would have been better to go with six cycles of TAC, but no data show six cycles are superior to four.
Early in the study we had several deaths in the ATC arm of B-30, probably due to the doses used — doxorubicin 60 mg/m2, docetaxel 60 mg/m2 and cyclophosphamide 600 mg/m2. We changed the doses to those used in Nabholtz’s regimen — doxorubicin 50 mg/m2, docetaxel 75 mg/m2, and cyclophosphamide 500 mg/m2 — and since then we’ve had very few deaths. We also changed the AT arm from doxorubicin 60 mg/m2 and docetaxel 60 mg/m2 to 50 mg/m2 and 75 mg/ m2, respectively. The TAC regimen produced a high rate of febrile neutropenia — about 29 percent in the metastatic setting and 23 to 24 percent in the adjuvant trial — which we felt was unacceptable, so we added growth factors. It is up to the investigators whether they use the long- or shorteracting growth factor.
— Sandra Swain, MD
Several clinical trials have addressed the benefit of taxanes in the adjuvant setting. The results from CALGB-9344 have been published and demonstrate an improvement in disease-free and overall survival with the addition of paclitaxel to AC chemotherapy. BCIRG- 001 — comparing TAC to FAC — also resulted in an improvement in diseasefree survival. Most recently, CALGB- 9741 documented an improvement in disease-free and overall survival with dose-dense AC and paclitaxel every two weeks with growth factor support.
Some physicians dismiss the findings from CALGB-9741, believing there is minimal clinical application of the results. I disagree. Increasing the frequency of administration of AC and paclitaxel from every three weeks to every two weeks, with filgrastim support, clearly resulted in a substantial improvement in disease-free survival. Interpretation of the results is controversial because CALGB-9741 was designed before the administration of weekly taxanes. Today, studies such as the Intergroup’s ECOG-N9831 — for patients with node-positive, HER2- positive disease — use weekly paclitaxel. We’ve seen a shift in the administration schedule of paclitaxel, and some physicians question whether the improvement in disease-free survival was due to increasing the density of paclitaxel, AC or both. That issue remains unresolved, but a dose-dense approach is an acceptable option for women with nodepositive early breast cancer.
— Vicente Valero, MD
The management of patients with node-positive breast cancer has become more complex in the last year, and we now have several very good regimens. However, we don’t have proof that any of these regimens is absolutely better than another. The options today include the FEC regimen, which is not commonly used in the United States, the TAC regimen and sequential AC followed by paclitaxel or docetaxel.
If I’m going to use AC followed by a taxane, I tend to use the dose-dense regimen published in the Journal of Clinical Oncology based on CALGB- 9741, or I may still use AC once every three weeks followed by weekly paclitaxel.
If I were to use docetaxel, then I would use AC once every three weeks followed by docetaxel once every three weeks, because of docetaxel’s tolerability when administered once every three weeks compared to weekly. When I use the AC every two-week regimen, I use pegfilgrastim rather than filgrastim. While we do not have data on that, I believe it is much more convenient for patients, and we have incorporated it into our clinical practice.
— Edith Perez, MD
In SWOG-S0221, the combination dose-dense arm of CALGB-9741 was selected for the initial randomization instead of the sequential arm. Our rationale was to shorten the duration of treatment and to make it more comparable to the AC regimen in the experimental arm.
In the second randomization, we were originally going to compare docetaxel alone to docetaxel plus capecitabine. We decided to compare paclitaxel every two weeks to paclitaxel every week for a couple of reasons. First, the docetaxel/ capecitabine combination is being investigated in several other multicenter adjuvant trials.
Second, it was felt that we should preserve the control arm from CALGB-9741, which administered paclitaxel every two weeks. At the end of SWOG-S0221, we hope we will know the optimal way to administer paclitaxel in the adjuvant setting.
— G Thomas Budd, MD
As a first- or second-line chemotherapy in patients with advanced breast cancer, Taxotere has significant antitumor activity, with response rates ranging from 44% to 68%. This impressive single-agent activity is better than that observed in historical control phase II trials of single-agent Adriamycin and is similar to the results obtained with the standard combination chemotherapy regimens including cyclophosphamide/ Adriamycin/fluorouracil (CAF); cyclophosphamide/ methotrexate/5-f lourouracil (CMF); and Adriamycin/cyclophosphamide (AC).
Importantly, studies involving Taxotere from the University of Texas at San Antonio, EORTC, and MD Anderson document the highest response rates yet observed in patients with anthracyclineresistant advanced breast cancer. This apparent non-cross-resistance suggests that a combination of Adriamycin plus Taxotere may be advantageous.
— NSABP-B-30 protocol, Rationale,
November 14, 2002 [Citations omitted]
EDITOR’S COMMENT
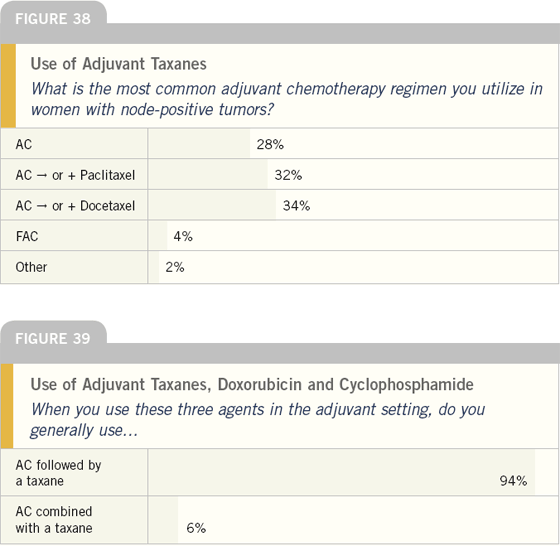
About two-thirds of physicians state that they generally use taxanes in node-positive cases. This contrasts to the actual case they described from their practice (see page 11, Figure 10) of a woman with an ER-positive, node-positive tumor, for whom the most common regimen used was AC.
TAC is the most common regimen used when taxanes are combined with AC, but AC followed by a taxane is by far the most frequent approach to delivering these agents.
Related Comments from Research Leaders
Two trials evaluating AC followed by paclitaxel have reported a significant improvement with that adjuvant regimen. The NSABP-B-28 trial, which added four cycles of paclitaxel to AC, had results similar to the earlier study. Many oncologists have substituted docetaxel for paclitaxel, and the Taxotere-311 data lend support to that in the adjuvant setting. In a younger patient with node-positive disease who is not eligible for a trial, I am more likely use AC followed by docetaxel. The study comparing docetaxel, doxorubicin and cyclophosphamide (TAC) to 5-fluorouracil, doxorubicin and cyclophosphamide (FAC) is a very clean trial. It is often interpreted as TAC being more effective for patients with one to three positive nodes, but not those with four positive nodes. However, that is the way the data were presented, and TAC is pretty effective across the board. Some oncologists have expressed concern about the TAC regimen’s toxicity, and it probably requires the use of growth factors.
— Stephen E Jones, MD
We’re participating in the Intergroup trial CALGB-40101, led by Larry Shulman, which asks, “Is AC for six cycles better than four cycles?” This study also attempts to determine whether anthracyclines are necessary or whether they could be replaced with a taxane to avoid the cardiotoxicity. It’s a four-arm study — AC for four cycles or six cycles every two weeks, or paclitaxel administered every two weeks for four versus six cycles. After the dose-density data were presented they decreased the timing from every three weeks to every two weeks, all with growth factor support.
— Julie R Gralow, MD
The TAC data were not surprising; I expected them to become positive for survival and disease-free survival. The analysis was very clear — no question — TAC is better than FAC. Now the question is: Is the dose-dense regimen, presented by Marc Citron last year, of AC every two weeks for four cycles with growth factors, followed by dose-dense paclitaxel for four cycles, better or worse than TAC?
The trial comparing TAC to FAC utilized an intravenous FAC regimen, but we’ve known for a long time that the SWOG FAC regimen is probably better. SWOG FAC uses daily oral cyclophosphamide, which prolongs its administration compared to the allintravenous regimen.
As established by randomized trials, classic CMF using oral cyclophosphamide is superior to an all-intravenous CMF regimen. Therefore it’s even more plausible that classic FAC would be better than the all-intravenous FAC regimen. Although TAC is better than intravenous FAC, it cannot be concluded that TAC is better than the SWOG FAC regimen.
— I Craig Henderson, MD
Next page
Page 1 of 2
|

